Venous ulcers occur in about 1% of the population but account for up to 70% of all leg ulcers. They are most common in people over the age of 50 and are more common in women than men.
Table of Contents
ToggleWhat are Venous Ulcers?
Venous ulcers are wounds that develop when the veins in your legs are not able to efficiently pump blood back to your heart. This can cause blood to Pool in your legs and ankles, leading to swelling (Known as edema). Over time, this can damage the skin and underlying tissue, eventually causing an ulcer.
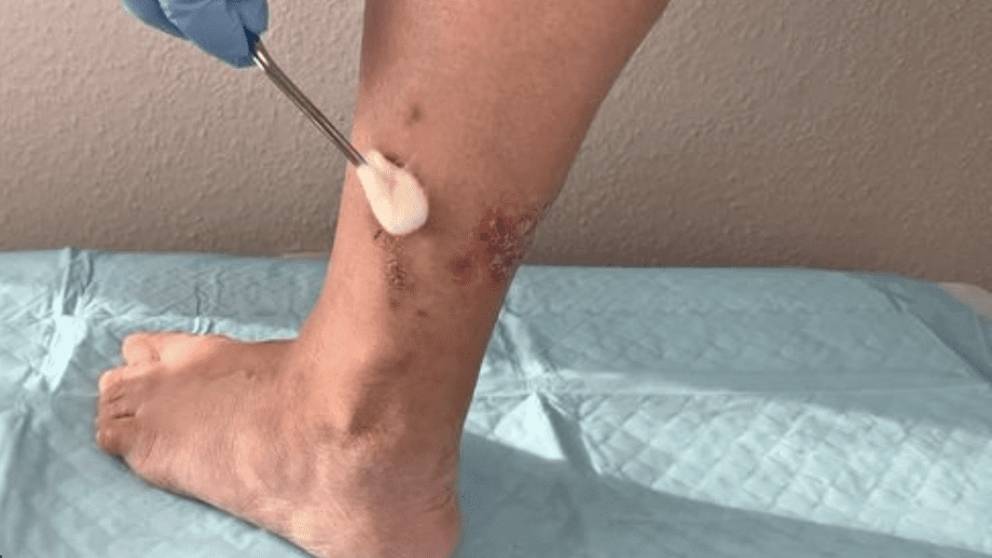
What are the Symptoms of Venous Ulcers?
The most common symptom of a venous ulcer is a dull ache or pain in the affected area. Other symptoms May include:
- Swelling in the leg
- Cramping or discomfort in the leg
- Itching or burning sensation on the skin over the affected area
- Red or discolored skin over the affected area
- Crusting or bleeding from the ulcer
Where are Venous Ulcers Found?
Venous ulcers usually develop on the inside of the leg, just above the ankle. They are shallow sores that May be painful, itchy or both. Venous ulcers often have a raised edge and a crusted or scabbed center.
If left untreated, venous ulcers can take weeks or even months to heal. In some cases, they may recur or become chronic (long-term).
What Causes Venous Ulcers?
Venous ulcers are wounds that occur when blood flow from the legs back to the heart is impeded and high pressure in the veins causes damage to the skin and underlying tissue. Venous ulcers are most common on the inner ankle, lower leg, or top of the foot.
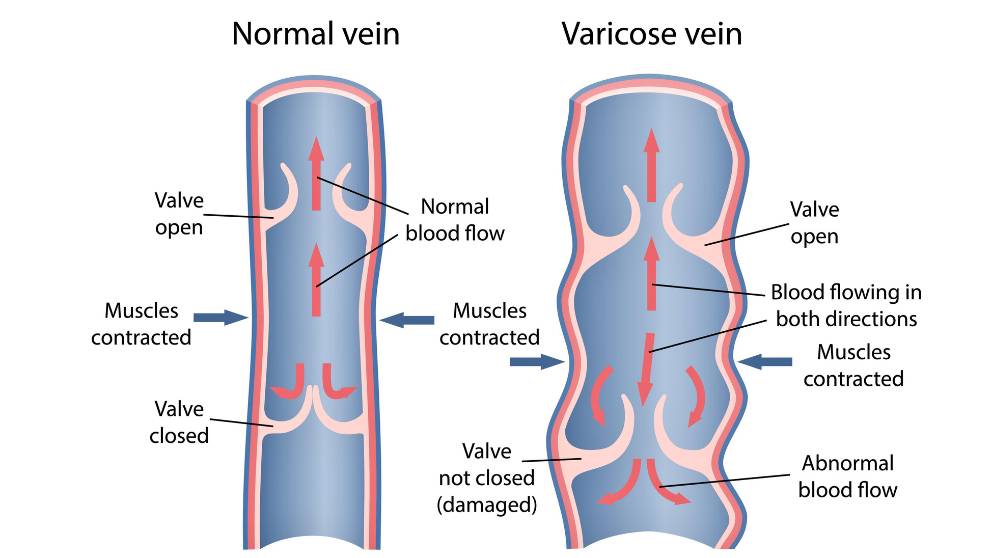
Chronic venous insufficiency results from valves in the veins that are not working properly. This allows blood to flow backward and Pool in the leg, which increases pressure and can damage the skin.= through causing ulcers
Other factors that May contribute to the development of venous ulcers include:
- Obesity
- Pregnancy
- Standing or sitting for Long periods
- Previous injury or surgery to the legs
- Heart failure
- Chronic (Long-term) Lung disease
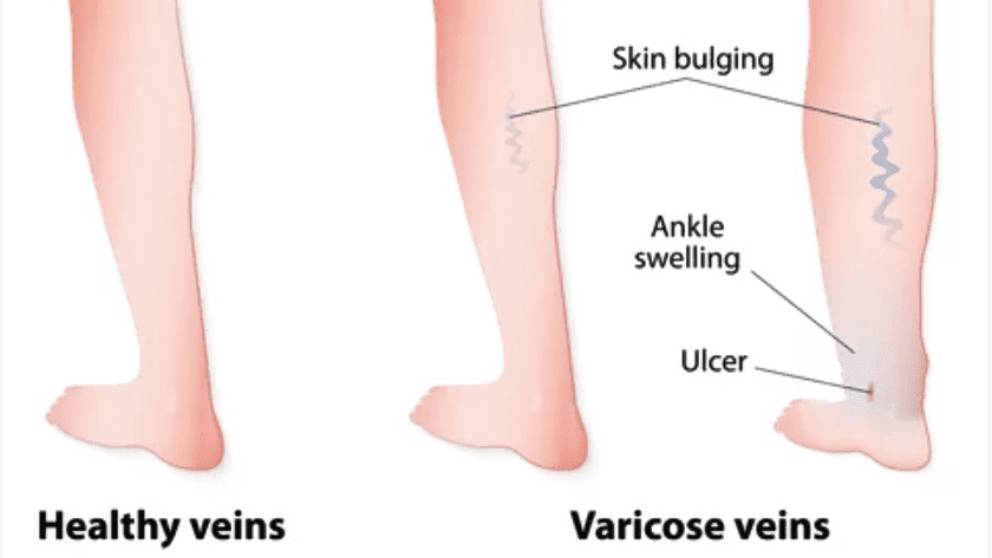
What are the Risk Factors for Venous Ulcers?
Several factors May increase your risk of developing venous ulcers, including:
- Age – venous ulcers are most common in people over the age of 50.
- Gender – women are more likely than men to develop venous ulcers.
- Family History – you May be more likely to develop venous ulcers if you have a family history of the condition.
- Varicose Veins – venous ulcers are more common in people with varicose veins.
- Smoking – smoking can damage the valves in your veins and make it harder for blood to flow from your legs back to your heart.
How are Venous Ulcers Diagnosed??
Your doctor Will likely start with a physical exam and a review of your medical history. Your doctor Will likely ask about your symptoms and whether you have any risk factors for venous ulcers, such as varicose veins or venous insufficiency. They May also order tests to check the blood flow in your legs or to rule out other conditions that could cause similar symptoms. They May also order one or more of the following tests:
Doppler Ultrasound: This test uses sound waves to create a picture of blood flow through your veins. It can help your doctor identify areas of blockage or damage.
Venogram: This test involves injecting a dye into your veins and then taking x-rays to track the dye as it moves through your veins. This can help your doctor identify blockages or damage.
CT Scan: This test uses x-rays and computer imaging to create detailed pictures of your veins.
MRI: This test uses magnetic fields and radio waves to create detailed pictures of your veins.
How Can I Prevent Venous Ulcers?
You can help prevent chronic venous ulcers by taking steps to improve blood flow in your legs and reduce pressure on your veins. Some things you can do to improve blood flow and reduce pressure include:
- Exercise regularly
- Maintain a healthy weight
- Avoid sitting or standing for Long periods
- Wear loose-fitting clothing
- Elevate your legs when you are sitting or lying down
Compression stockings apply gentle pressure to your legs and help improve blood flow. Your doctor May recommend that you wear compression stockings if you have varicose veins, venous insufficiency, or other conditions that can cause venous leg ulcers.
How are Chronic Venous Ulcers Treated?
The goal of treatment for venous ulcers is to promote healing, relieve pain, and to prevent a recurrence. Treatment for venous ulcers usually involves a combination of self-care measures and medical interventions.
What are the Self-Care Measures You Can Do for Venous Ulcers?
Self-care measures May include:
Elevating the Affected Leg: This can help reduceswelling and improve blood flow.
Wearing Compression Stockings: These garments apply pressure to your legs and help promote blood flow.
Cleaning The Wound: This helps prevent infection and promotes healing. Your doctor Will likely prescribe a special cleaning solution for you to use.
Applying Bandages:This helps keep the wound
Compression Therapy: Compression stockings or bandages are used to help reduce swelling and improve blood flow in the affected leg.
Leg Elevation: Keeping the affected leg elevated above heart level
What are the Medical Interventions for Venous Ulcers?
Medical interventions for venous ulcers May include:
Antibiotics: These medications are used to treat or prevent infection.
Pain Relief Medication: These medications can help relieve pain and inflammation.
Wound Dressings: These are used to protect the wound and promote healing. Your doctor Will likely prescribe a specific type of dressing for you to use.
Debridement: This is a procedure in which dead or infected tissue is removed from the wound. It can help promote healing.
What Surgical Procedures May Be Indicated for Venous Ulcers?
Surgical procedures for venous ulcers May include:
Vein Surgery: This can help improve blood flow in the affected leg by removing varicose veins (Vein ligation and stripping,phlebectomy)
Skin Grafting: This is a procedure in which healthy skin is taken from another area of your body and transplanted to the wound. It can help improve healing.
Amputation: In some cases, amputation May be necessary if the ulcer does not heal with other treatments.
What are the advanced non-surgical methods used to treat venous ulcers?
Advanced non-surgical methods that are used to treat venous ulcers include:
Hyperbaric Oxygen Therapy: This is a treatment in which you breathe 100% oxygen while inside a chamber. It can help improve healing.
Negative Pressure Wound Therapy: This is a treatment in which a vacuum pump is used to remove air from the wound. It can help promote healing.
Treatment of chronic venous insufficiency which involves treating varicose veins such as:
How do imaging & interventional specialists determine whether you could benefit from advanced, non surgical treatment for your venous ulcers?
After a review of your medical history, a physical exam May be performed. If needed we Will talk with other members of your care Team and analyze your medical chart to determine what treatment plan best fits your clinical situation.
After a complete evaluation has been performed, the diagnosis, chronicity, and severity of your venous ulcers are determined then an imaging & interventional specialist Will discuss the best treatment options for you.
Why Choose Imaging & Interventional Specialists?
Imaging & interventional specialists are leaders in interventional radiology and experts in the non-surgical procedures that Will address your venous ulcers.
Our physicians perform “PINHOLE” procedures every day offering this region’s leading, world-class, state-of-the-art solutions for venous ulcers. Our non-surgical image-guided procedures are cutting-edge technology without the cutting, without the scalpel. You leave with a band-aid!
At imaging & interventional specialists board-certified physicians offer in-house testing for diagnosis and to develop an individualized treatment program for your venous ulcers.

